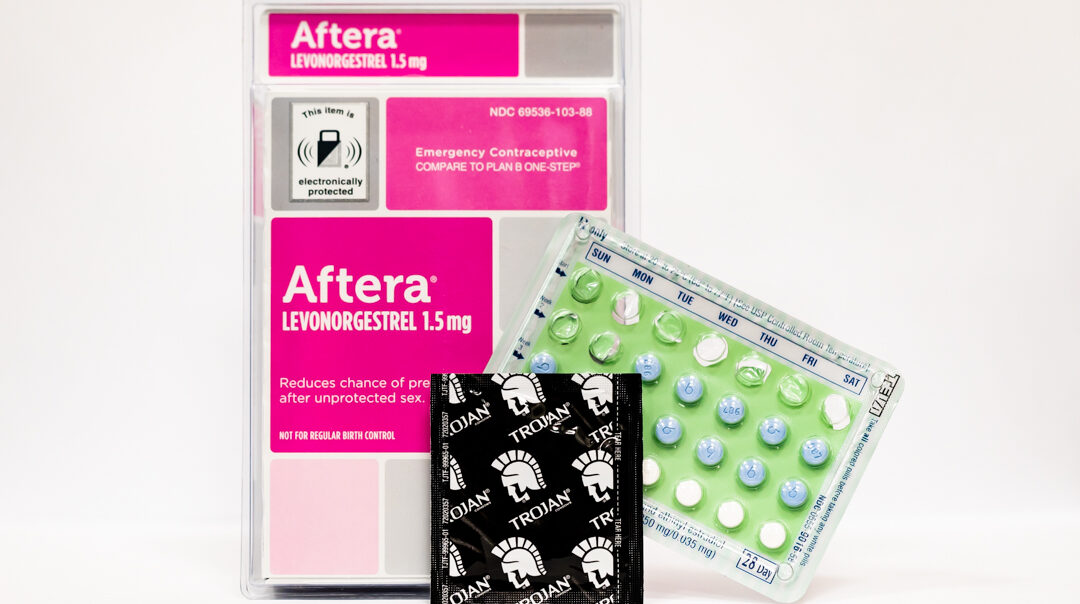
There are many contraceptive options available. Photo by Lauren Hough.
ALLIE MCKIBBEN | STAFF REPORTER | amckibben@butler.edu
Modern birth control was first invented in 1914, and made FDA approved within the United States in 1960 with the help of activist Margaret Sanger. Its invention has reduced child poverty, lowered public spending on health amenities, pushed back on disparities for disadvantaged populations and so much more.
Birth control also plays an important role in the advancement of people who menstruate in the workplace, as it supports them in deciding when, and if, they want to have children. With the Supreme Court deciding to overturn Roe v. Wade this summer, access to birth control has become a concern for people across America.
The CDC found in a study done from 2017 to 2019 that 65.3% of women aged 15-49 were using some form of contraception. For Julia Fryrear, a junior sociology and criminology combined major, it has been an essential asset in regulating her menstrual cycle and acne.
“[Birth control] allows me to feel a lot more confident about myself, and … it’s something that I know is reliable as long as I keep taking it,” Fryrear said. “Not only will my acne be better, but it also will make sure that I know when my period is coming.”
Yet, Fryrear does not know the specifics of how birth control functions. Fortunately, Dr. Veronica Vernon, assistant professor of pharmacy practice, is knowledgeable on the subject and has the answers. Vernon has been a practicing pharmacist for over a decade in the state of Indiana and helps train healthcare professionals across the country on how to use different methods of contraception. She assures that although there are birth control options that are more popular, there is such a wide variety that there is a method for everyone.
According to the CDC, behind permanent sterilization, the oral contraceptive pill is the most used contraceptive among women in the U.S. at 14%, followed by long-acting reversible contraception at 10.4% and the condom at 8.4%.
The oral contraceptive pill, or just “the pill,” works by taking a daily pill that distributes hormones through the body to prevent pregnancy. The pills are usually prescribed in packs of 28 pills, one per day for four weeks, along with a week of placebo pills during which a period takes place. Placebo pills are non-hormonal pills that allow users to get a period for that week, but users can skip the week of placebo pills to avoid having a period altogether.
“The [progesterone in combined oral contraceptives] is to prevent ovulation from occurring, and the [estrogen is to] thicken the cervical mucus,” Vernon said. “ … When [the mucus] gets thick, the sperm can’t get through that mucus, and the sperm gets trapped and dies and then gets removed from there.”
Along with preventing pregnancy, Vernon said the pill can also help control the predictability and the heaviness of people’s menstrual periods. Also, depending on what type of progesterone is used in the pill, oral contraception can help manage acne.
The second most used birth control within the U.S. are long-acting reversible contraceptives, LARCs. The most commonly used birth control within LARCs are the intrauterine devices, or IUDs. IUDs are T-shaped and can be about the size of a quarter. They last between three and 10 years and are inserted into the cervix with a string attached, which helps physicians remove them. The two types of IUDs, progesterone-only and copper, give people options with whether they want a form of contraception that utilizes hormones or not.
The copper IUD can also be used as emergency contraception if placed up to five days after unprotected sex. Vernon states that 80% of people who use it like emergency contraception keep the IUD in for up to 10 years after insertion.
Other types of emergency contraception include the morning after pill, most commonly referred to by the brand name Plan B. It can also be referred to by its competitor ella which also acts as emergency contraception, but is a different drug. This pill prevents ovulation, when the mature egg is released into the ovaries, which then prevents the fertilization of the egg. This contraceptive method is most commonly used after unprotected sex as a safety net but can only be effective within a few days of unprotected sex. It does not cause termination of a pregnancy.
“Plan B is over-the-counter,” Vernon said. “That’s just one pill taken one time. It’s best if you can take it as soon as possible, like within 24 hours of unprotected intercourse. It is effective up to 72 hours — or three days — after unprotected intercourse. It can be used up to five days, but it’s less effective in that three to five day window.”
Although emergency contraception is convenient, the efficacy may depend on the person or drug. Vernon points to how studies show mixed results in the effectiveness of Plan B on people who weigh over 165 pounds.
“I tell people that if there is [ella] — which is prescription only — available, it may be more effective [than Plan B],” Vernon said. “However, if this is not an option, or the copper IUD is not an option at the time for someone, then Plan B is completely acceptable to use.”
The implant and the shot release the same exact progesterone hormone that prevents ovulation; the difference is one is implanted in the body, and one is delivered as a shot.
The implant is a small, flexible rod that is placed in the upper arm and releases a low dose of hormones into the person’s bloodstream. It can be removed at any time, but it lasts for about three years.
Medroxyprogesterone acetate, or “the shot,” is an injection taken every three months. The most commonly used brand is Depo-Provera as they have two different shots to choose from. The first option, the original Depo-Provera shot, is inserted deep into the muscle, usually the upper arm or butt cheek. The second option, the Depo-SubQ Provera 104, does not need to go as deep, and is administered in the upper thigh or stomach. Vernon notes that both Depo shots do not have to be administered in a doctor’s office and can be done at home.
All five — the oral contraceptive pill, the IUD, the implant, the shot and the morning after pill — have some of the highest recorded birth control efficacies. According to Vernon, the oral contraceptive pill’s failure rate is about 9%, the morning after pill’s is 5% within the three day window and the IUD’s is 0.2%.
An important difference between the oral contraceptives and the other birth control methods is that the others do not have estrogen in them, so according to Vernon, they have far fewer side effects and reasons why someone would be unable to take it.
However, there are notable side effects in all of these methods of birth control, such as nausea and breast tenderness, which improve over several months, along with breakthrough bleeding, which can last up to 12 months for some people.
She also stresses that estrogen can make people more at risk for blood clots and migraines, so considering this, people who have unusually high blood pressure or migraines with aura, might want to steer away from estrogen-based birth controls.
Due to the fact that there are side effects and that birth control can change people’s bodies, many individuals choose not to pursue birth control at all. Although the most effective methods of birth control are the hormonal, Vernon points out that there are other effective non-hormonal birth controls that individuals can seek out, such as diaphragms, condoms and fertility awareness-based methods.
Although birth control is used more by women than any other demographic, Vernon stressed that the conversation of birth control needs to be more inclusive.
“We often talk about this for women, but it’s for anyone with a uterus and ovaries that wants to prevent pregnancy,” Vernon said. “So this is important that we ensure that we’re including gender diverse and transgender folks in this discussion too.”
Vernon recommends that individuals meet with their physician to find the version of birth control that best suits their wants and needs. She said she understands everyone has different circumstances, so talking to parents or guardians may not be the right choice for everyone. But, Vernon confirms that the HIPAA act protects patients’ personal health information from outside parties.
“I don’t want to deter anyone from having these conversations, but I think it’s important to know what your rights are as a patient under the Health Information and Patient Affordability Act, or HIPAA,” Vernon said. “Your health information is your health information. So who you choose to … share it with is your decision, not your medical provider’s.”
In Indiana, only doctors, physician assistants and nurse practitioners can provide a prescription to birth control; pharmacists cannot. Vernon stressed that Health Services provides birth control on campus, available for all students.
Director of Health Services Maxie Gardner said Health Services has many types of birth control: the oral contraceptive pill, various types of IUDs, the morning after pill, the implant, the Depro-Vera shot and condoms. Gardner stresses the accessibility of birth control Health Services provides and implores students to take advantage of this resource on campus.
To further the accessibility of birth control on Butler’s campus, Gardner was elated to announce that Butler will be installing a health-related vending machine that serves emergency contraception.
“ … We’re very excited about what’s new and coming to Butler, and we are looking at having a vending machine located in Atherton where students have 24/7 access to emergency contraception, as well as condoms and other health care items that [students] might run out of in their dorm rooms, such as ibuprofen and cough drops and cold medicine,” Gardner said. “ … My hope is that we will have that here on campus by December, and all of the leadership here at Butler is extremely supportive of this.”
Gardner said there will be Plan B and a generic morning after pill in the vending machine, which will allow students to have different pricing options. Plan B costs around $45 to $50 whereas the generic brand costs around $13 to $15.
Until the vending machine is installed, individuals can still get emergency contraception at Butler’s Health Services, no appointment needed.